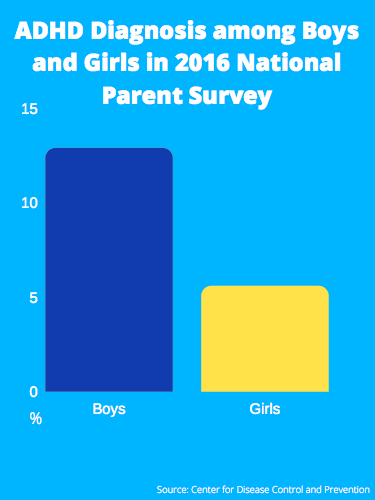
In an op-ed last week in the New York Times entitled “Diagnosis: Human,” contributor Ted Gup made a case against over-medicating those diagnosed with mental health disorders. He cited concerns about the high number of school-age kids diagnosed with attention deficit hyperactivity disorder to make the larger point that we are in an environment that too easily encourages medication when diagnosed. Gup has these concerns input because his son died of drug abuse.
The timing of this op-ed seemed to be fitting, as this week is Mental Health Awareness Week. Established by Congress in 1990, Mental Health Awareness Week was designed to educate and increase awareness about mental illness. We are glad this week has a place on campus, and we hope this conversation will open up a lasting dialogue, because it still has work to do. While it is great that many of the stigmas surrounding mental illness have been eliminated, there are issues surrounding medication that remain to be addressed.
In a Sept. 20, 2012 article in the Tribune, Michael Zebrowski, the director of the Marquette Counseling Center, expressed a concern about medication.
“In some ways, pharmaceutical companies may educate about and destigmatize psychiatric medications more than other agencies,” Zebrowski said in an email. “But I do get concerned that people diagnose themselves, decide what might be a good medication for them based on little information, and then request it of their doctor.”
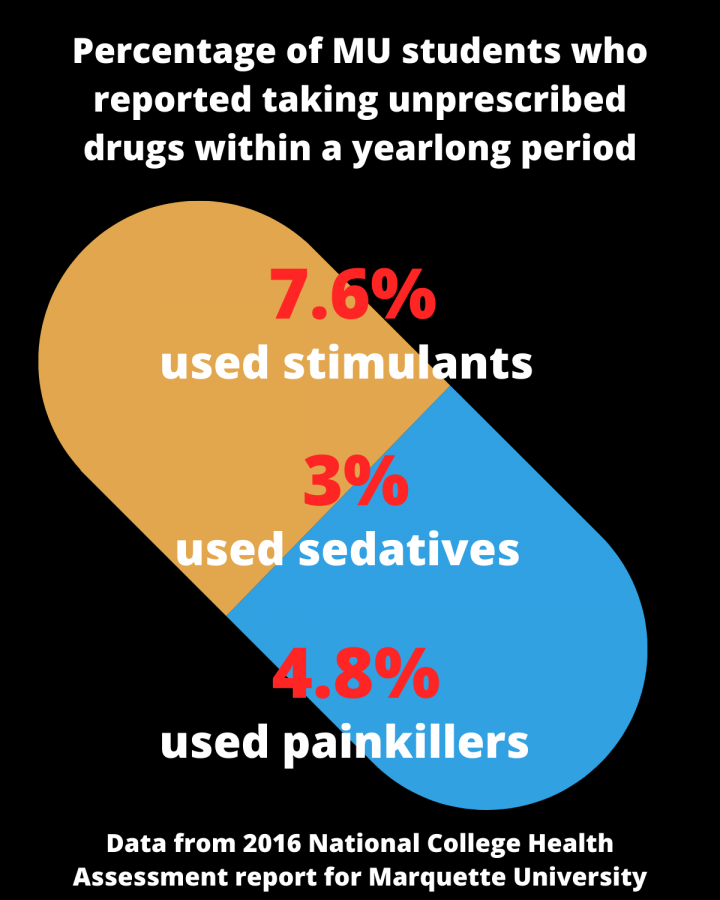
We share that concern. Using nonprescribed Adderall to improve study habits is a generally accepted phenomenon at Marquette and other college campuses around the country. This contributes to a culture of exploiting medication and its availability for any use desired. Even Gup’s son was selling his medication to undiagnosed friends before he died, according to the Times piece.
Mike Haen, a senior in the College of Arts & Sciences and a leader in the Mental Health Awareness Week planning, said educating students about appropriate responses to discussions of possible illness or suicide can be beneficial on a college campus. He likened the situation to that of a broken arm. If someone were to see you in a cast, he said, they would ask what they can do to help, whereas if a friend confesses emotional distress or a diagnosis of a mental illness, the respondent usually does not know how to answer.
Haen said the best response is to convey your support for the person and ask questions such as, “Who are you seeing for treatment?” and “How can I help you?”
An academic panel held Monday night, “Mental Health in the Academy,” featured a presentation by biomedical sciences professor and associate chair David Baker, who pointed out that medicine for illnesses such as schizophrenia has not evolved much since the late 1800s. This alone shows that alternative treatment options must be considered.
Current medication often only addresses some issues and includes negative side effects. While a prescription can help control symptoms, medicine cannot solve personal conflicts or other very real tensions that can contribute to mental illness. Those issues, rather, must be addressed through counseling or therapy.
Holistic care is also not only for those with a diagnosed illness. Anyone dealing with a difficult time, such as grief over the loss of a loved one, does not need to turn to a pill for comfort. And as Gup pointed out, using medication as a form of escapism can in fact inhibit our ability to come to grips with grief.
“Challenge and hardship have become pathologized and monetized,” Gup wrote. “Instead of enhancing our coping skills, we undermine them and seek shortcuts where there are none, eroding the resilience upon which each of us, at some point in our lives, must rely.”
We fully recognize the benefit and necessity of medication to treat mental illness, and we are grateful for efforts to destigmatize it. We encourage our Marquette community, however, to be open to dialogue on emotional concerns, as well. Regardless of whether feelings of sadness or worry constitute a diagnosis for mental illness, it is important to acknowledge and discuss them. Similarly, the Counseling Center is not only for those with “problems.” It is actually very healthy to seek help when needed. Asking for help when needed is a sign of strength.
Mental Health Awareness Week and other similar outreaches are valuable. They have contributed to the destigmatization of mental illnesses and will continue to do so. This week, though, should also focus on the medications used to treat illnesses, their positive and negative effects and how their use contributes to a culture that often seems afraid to address genuine human emotion.